Reporting Patient Incidents: A Best Practices Guide | i-Sight
24 hours ago · What is a Patient Incident Report? A patient incident report, according to Berxi, is “an electronic or paper document that provides a detailed, written account of the chain of events leading up to and following an unforeseen circumstance in a healthcare setting.” Reports are typically completed by … >> Go To The Portal
Instead, the nurse should make a complete and separate entry regarding the incident in the patient’s chart. Incident reports are reviewed by nurse supervisors or managers, or sometimes by a panel who will decide on whether to investigate further.
Full Answer
What is a patient incident?
As defined by Berxi, a patient incident report is “a detailed, written description of the chain of events leading up to and following an unforeseen scenario in a healthcare context,” which can be either computerized or paper-based. Nurses or other qualified professionals are often responsible for completing reports.
How to write a good accident or incident report?
- The type of incident that took place
- Where the incident happened
- The date, day and time of the incident
- Names of the people involved
- Injuries that were obtained
- Medical treatment that may have been required
- Equipment that was involved
- Events leading up to the incident that could have contributed to it taking place
What is a hospital incident report?
The man has not been identified. Medical staff at the hospital told investigators that the man's injuries were not consistent with a traffic accident. The incident report indicates that the man was injured by a gunshot. However, the official cause of death ...
What is a patient safety incident report?
Report a patient safety incident Patient safety incidents are any unintended or unexpected incident which could have, or did, lead to harm for one or more patients receiving healthcare. Reporting them supports the NHS to learn from mistakes and to take action to keep patients safe.
Do you put incident report in chart?
All Information in its Proper Place Record clinical observations in the chart—not in the incident report—and make no mention of the incident report in the patient record. The report is a risk management or administrative document and not part of the patient's record.
How do you document an incident report?
What Does an Incident Report Need to Include?Type of incident (injury, near miss, property damage, or theft)Address.Date of incident.Time of incident.Name of affected individual.A narrative description of the incident, including the sequence of events and results of the incident.Injuries, if any.More items...•
How is an incident report recorded in the patient's medical record?
- The incident report is filed separately from the medical record with the original usually being sent to the legal counsel for the facility and a copy stored in the Quality Assessment Department or the Risk management department.
What should you not document in a patient's chart?
7 Common Pitfalls to Avoid in Charting Patient InformationFailing to record pertinent health or drug information. ... Failing to document prior treatment events. ... Failing to record that medications have been administered. ... Recording on the wrong patient's chart. ... Failing to document discontinuation of a medication.More items...
What is incident report in hospital?
In a health care facility, such as a hospital, nursing home, or assisted living, an incident report or accident report is a form that is filled out in order to record details of an unusual event that occurs at the facility, such as an injury to a patient.
What are the 4 types of incident reports?
Common Types of Incident ReportsWorkplace. Workplace incident reports detail physical events that happen at work and affect an employee's productivity. ... Accident or First Aid. ... Safety and Security. ... Exposure Incident Report.
What information should be documented in an incident log?
The incident log documents all details about an event, including date, time, what happened, who was involved and who witnessed the event. You should fill out the incident log immediately after an incident.
What do you do with an incident report once it is completed?
What do you do with an incident report once it is completed? Give it to the appropriate supervisor. Why should you initiate an incident report on an event that only has a risk for injury?
When should a incident report be completed?
Generally, you should complete an incident report whenever an unexpected occurrence causes property damage or personal injury.
How do you document a patient chart?
Tips for Patient ChartingUse Evidence-Based Care Plans. ... Document Patient Care Using Standard Medical Terminology. ... Avoid Using Restricted Abbreviations in Patient Charting. ... Save Time by Integrating Technology. ... Use the HER's Dictation Functionality. ... Document to Medical Necessity.More items...•
Which information should be included in patient documentation?
What should be documentedThe most current information. ... Clinically pertinent information. ... Rationale for decisions. ... Informed Consent discussions or the patient's refusal of care. ... Discharge instructions. ... Follow-up plans. ... Patient complaints and response. ... Clinically pertinent telephone calls.More items...
What are the basic rules of documentation?
Be clear, legible, concise, contemporaneous, progressive and accurate. Include information about assessments, action taken, outcomes, reassessment processes (if necessary), risks, complications and changes.
How Effective Are Incident-Reporting Systems for Improving Patient Safety?
It is possible to acquire information on patient safety occurrences through the use of incident-reporting systems (IRSs). Even if they come with a...
When to Report an Incident to the Police?
The general rule of thumb is that an incident report should be completed as quickly as possible after an occurrence happens. Minor injuries should...
How Are Patient Safety Event Reporting Systems used?
Hospitals are replete with patient safety event reporting systems, which serve as a cornerstone of efforts to detect patient safety incidents and q...
How to write an incident report?
In determining what to include in an incident report and which details can be omitted, concentrate on the facts.#N#Describe what you saw when you arrived on the scene or what you heard that led you to believe an incident had taken place. Put secondhand information in quotation marks, whether it comes from a colleague, visitor, or patient, and clearly identify the source.# N#Include the full names of those involved and any witnesses, as well as any information you have about how, or if, they were affected .#N#Add other relevant details, such as your immediate response—calling for help, for example, and notifying the patient’s physician. Include any statement a patient makes that may help to clarify his state of mind, as well as his own contributory negligence.#N#It’s equally important to know what does not belong in an incident report.#N#Opinions, finger-pointing, and conjecture are not helpful additions to an incident report.#N#Do not:
When is an incident report required?
When a situation is significant—resulting in an injury to a person or damage to property —it’s obvious that an incident report is required. But many times, seemingly minor incidents go undocumented, exposing facilities and staff to risk. Let’s discuss three hypothetical situations.
Why is it important to fill out incident reports?
Filing incident reports that are factually accurate is the only way to help mitigate potentially disastrous situations arising from malpractice and other lawsuits. It’s your responsibility to record unexpected events that affect patients, colleagues, or your facility, regardless of your opinion of their importance.#N#If the incident report has been filled out properly with just the facts, there should be no reason to be concerned about how it’s used. The danger comes only when incident reports contain secondhand information, conjecture, accusations, or proposed preventive measures that do not belong in these reports.
Why is incident reporting important?
An incident report invariably makes its way to risk managers and other administrators, who review it rapidly and act quickly to change any policy or procedure that appears to be a key contributing factor to the incident. The report may also alert administration that a hospital representative should talk to a patient or family to offer assistance, an explanation, or other appropriate support. That’s an important function because such communication can be the balm that soothes the initial anger—and prevents a lawsuit.
What happens when incident reports are filled out properly?
If the incident report has been filled out properly with just the facts, there should be no reason to be concerned about how it’s used. The danger comes only when incident reports contain secondhand information, conjecture, accusations, or proposed preventive measures that do not belong in these reports.
What is not a good addition to an incident report?
It’s equally important to know what does not belong in an incident report. Opinions, finger-pointing, and conjecture are not helpful additions to an incident report. Do not: Offer a prognosis. Speculate about who or what may have caused the incident. Draw conclusions or make assumptions about how the event unfolded.
How to protect yourself and your patients?
Protect yourself and your patients by filing incident reports anytime unexpected events occur . If you’re the one who discovers the incident, or you have been involved in the situation leading up to it and know more about it than your colleagues, filling out an incident report is your responsibility.
What Is Patient Incident Report?
Medical events can occur for a variety of reasons. Simply put, the medical system views each incident to be something that poses a threat to the health of patients or medical staff members in some way. “Incident Reporting in Healthcare,” as described in the realm of healthcare, is defined as the process of obtaining incident data and accurately presenting it for action. A newly discovered problem is recognized in order to aid in the identification and correction of the mistakes that occur. An incident report can be filed by a designated staff member (someone who has been granted permission to file reports) or by an employee who has witnessed the incident firsthand. The majority of the time, a nurse or other staff member will file a report within 24 to 48 hours of the incident occurring. It is preferable to capture and document an occurrence as soon as it occurs in order to achieve the best possible outcome.
What is the best way to write a patient incident report?
For example, employing precise and simple language will make the inquiry process more efficient and less time-consuming overall. Additionally, appropriate grammar, spelling, and punctuation should be used. Grammar errors can distort the interpretation of details contained within the report, making it more difficult to conduct an investigation into the incident.
What is a negative incident?
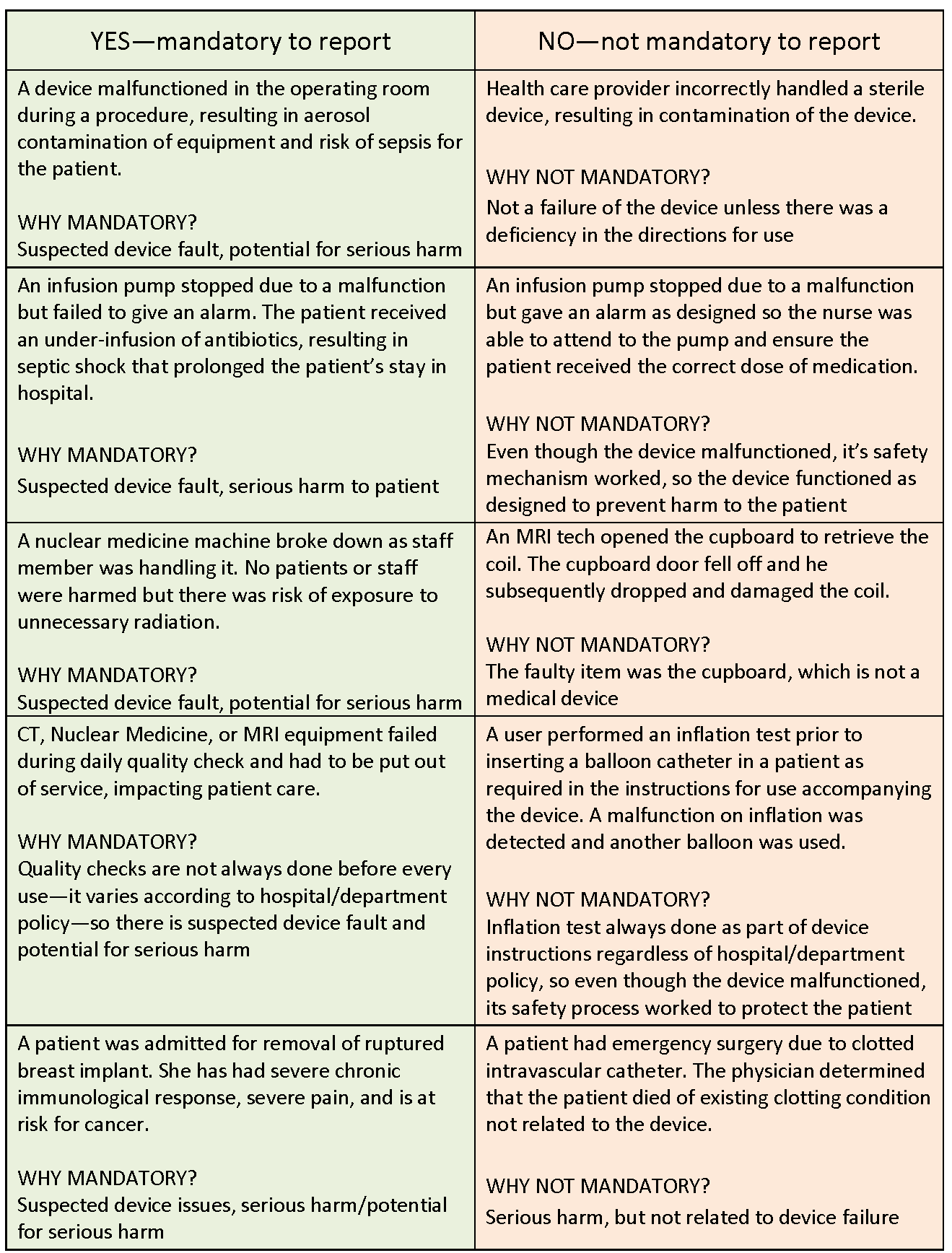
A Negative Occurrence: The effect of a detrimental incident is the injury or illness of a patient or another individual. It is possible for a patient to tumble out of bed and break their arm, or for a nurse to scratch them when she is taking their temperature. Missed the Mark by a Hair: A near miss occurs when there was a possibility for injury to a patient or when another person was on the verge of being harmed, but the situation was rectified before the harm could occur. For example, a patient may be apprehended while attempting to leave the facility early or may trip, but a nurse will grab them before they are injured. An incident with No Harm: A no-harm occurrence occurs when something happens to a patient or to another person, but no observable injury or illness results as a result of the event. For example, a patient may be given a blood transfusion intended for another patient, but no harm is done because the blood is compatible with the other patient.
What is incident reporting?
Incident reporting is usually used as a catch-all word for all-volunteer patient safety event reporting systems, which rely on persons who are directly involved in the events to provide specific information about what happened.
Why is incident reporting important?
The ultimate purpose of incident reporting is to improve the safety of the patient. By promoting higher safety standards and decreasing medical errors, incident reporting helps you create a more stable environment for your patients to flourish in. When your hospital provides high-quality patient care over time, it will eventually develop a positive reputation.
Why do medical incidents go unreported?
When an occurrence results in a person’s harm or property damage, it is necessary to file an incident report. Unfortunately, for every medical error that is recorded, there are about 100 other errors that go undetected. There are a variety of reasons why medical accidents go unreported, but one of the most common is a lack of knowledge on when to file a report.
How can hospitals improve their efficiency?
It is also possible to improve the efficiency of healthcare operations by using reporting tools. Hospitals can keep themselves out of legal issues by acquiring and evaluating incident data on a daily basis. A comprehensive medical error study analyzed the medical systems of 17 countries in Southeast Asia and investigated how inadequate reporting raises the cost burden on healthcare institutions and providers.
What is clinically pertinent information?
The medical record is a primary mechanism for providing continuity and communication among all practitioners involved in a patient's care. To gauge adequacy of your patient's medical records, consider what you would want documented if you were assuming management of the care of a patient you did not know.
What to include in a patient complaint?
Include copies of all clinically-related correspondence from and to patients, as well as notes from phone conversations and office discussions.
What is the importance of complete medical records?
Current, complete records which assist diagnosis and treatment, and which communicate pertinent information to other caregivers also provide excellent records for risk management purposes. The use of encounter forms, checklists, flowsheets, and computer-assisted documentation for high volume activities can save time and may also reduce the communication problems and errors caused by illegible handwriting. Missing, incomplete, or illegible documentation can seriously impede patient care and the defense of a malpractice claim, even when the care was appropriate. The following advice on documentation includes issues identified through analysis of malpractice claims.
Why is it important to keep your medical records up to date?
Keep your records up-to-date in order to provide the best resource for patient care and evidence that appropriate and timely care was provided. Clinically pertinent information. The medical record is a primary mechanism for providing continuity and communication among all practitioners involved in a patient's care.
What is current complete records?
Current, complete records which assist diagnosis and treatment, and which communicate pertinent information to other caregivers also provide excellent records for risk management purposes.
What should not be documented in Massachusetts?
What should not be documented. Derogatory or discriminatory remarks. In Massachusetts, patients have the right to access both office and institutional medical records and may be sensitive to notes they view as disrespectful or prejudicial. Include socio-economic information only if relevant to patient care.
What does medical records reflect?
Medical records often reflect differing diagnoses and treatment recommendations among multiple caregivers. However, oral or written criticism of previous health care contributes nothing to the patient's needs. Patients may take casual remarks critical of prior care quite seriously, possibly destroying their relationships with previous caregivers and/or you.
When To Write Incident Reports in Hospitals?
When an event results in an injury to a person or damage to property, incident reporting becomes a must. Unfortunately, for every medical error, almost 100 errors remain unreported. There are many reasons for unreported medical incidents, but not knowing when to report is one of the most common ones.
Who Prepares Incident Reports in Healthcare Facilities?
At QUASR, we believe all staff (and patients, too) should be able to report incidents or potential incidents they have witnessed. But in practice, it is a bit different. Some hospitals have designated persons who are authorized to file the reports. In some other hospitals, the staff usually updates their supervisor about an incident, then can file the report.
What is an incident in healthcare?
An incident is an unfavourable event that affects patient or staff safety. The typical healthcare incidents are related to physical injuries, medical errors, equipment failure, administration, patient care, or others. In short, anything that endangers a patient’s or staff’s safety is called an incident in the medical system.
Why is incident reporting important?
Improving patient safety is the ultimate goal of incident reporting. From enhancing safety standards to reducing medical errors, incident reporting helps create a sustainable environment for your patients. Eventually, when your hospital offers high-quality patient care, it will build a brand of goodwill.
What is clinical risk management?
Clinical risk management, a subset of healthcare risk management, uses incident reports as essential data points. Risk management aims to ensure the hospital administrators know their institution performance and identify addressable issues that increase their exposure.
What are near miss incidents?
#2 Near Miss Incidents 1 A nurse notices the bedrail is not up when the patient is asleep and fixes it 2 A checklist call caught an incorrect medicine dispensation before administration. 3 A patient attempts to leave the facility before discharge, but the security guard stopped him and brought him back to the ward.
How much of healthcare is wasted?
Even the World Health Organisation (WHO) has estimated that 20-40% of global healthcare spending goes waste due to poor quality of care. This poor healthcare quality leads to the death of more than 138 million patients every year. Patient safety in hospitals is in danger due to human errors and unsafe procedures.
Can you document an incident report in PT chart?
NEVER supposed to document in pt's chart that an incident report was completed...I would ask your instructor about this.
Can you report an incident in nursing notes?
NEVER, NEVER, NEVER mention that an incident report was filled out in your nursing notes! That leaves it wide open for that incident report to be subpenoed in a court case.
Can an incident report be brought in as evidence?
The incident report cannot be brought in as evidence unless it's noted in the chart. So no note...no incident report. I know to me it sounds kind of crappy because it seems to protect the hospital and could cause "harm" to the pt if there is a suit...but policy is policy. This policy may cover my butt sometime.
Is an incident report considered an internal investigation?
Your incident report is considered an internal investigation document. You should never document in your nurses notes that an incident report was completed. If you do, your report may be used in court. They are only to be used internally to investigate the incident.
What is incident report?
An incident report (also called an event report or occurrence report) is a formal report written by practitioners, nurses, or other staff members. It serves two purposes: * to inform facility administrators of incidents that allow the risk management team to consider changes that might prevent similar incidents.
What to do if incident is directly involved patient?
If the incident directly involved a patient, notify the healthcare provider .
What to do if a patient is injured in another department?
If your patient is injured in another department, it's up to the person who witnessed the incident in that department to write the incident report.
How to write a patient fall?
Write objectively. Describe exactly what you saw. If you didn't see the patient fall, document that you found the patient lying on the floor. Then document your actions, such as assessment of the patient for injury, assisting the patient back to bed, and calling the healthcare provider.
What should be included in a medical record?
The medical record documentation, completed close to the time of the incident report, should contain only factual, objective, descriptive documentation relative to the patient's condition and response to the incident. Never try to hide or cover up a mistake.
Why is it important to document what happened right away?
Because memories fade relatively quickly after an event occurs and critical components may be forgotten, it's vital to document what happened right away. An incident report is factual and complete; it doesn't include excuses for behavior or actions. The incident report is not a part of the patient's medical record.
Is an incident report a part of a patient's medical record?
The incident report is not a part of the patient's medical record. In most courts, the incident report is protected from discovery by the opposing attorneys. If you document the incident report in the patient's medical record, you've lost that protection.
What is the nurse violating in the Wright case?
Let's assume that Mr. Wright gets into a physical altercation with his roommate, Mr. Robinson. The nurse is violating Mr. Robinson's confidentiality if she documents his name anywhere in Mr. Wright's medical record, and vise versa. To get around this issue, employ a vague description such as 'the roommate' or the 'patient in bed A.'.
Why should nurses not chart assessments?
Nursing staff should never chart assessments, medication administration or treatments prior to actually completing the tasks because this may contribute to an inaccurate record filled with incorrect data. If the medical record contains nursing care that was never performed, this is fraudulent in some cases. Always remember that other clinicians may depend on correct documentation to assist in formulating decisions regarding patient care.
What should NOT be included in a nursing note?
The medical record is a permanent collection of legal documents that should supply an all-encompassing, accurate report concerning a patient's health condition. Physicians, nurses, social workers, dieticians, mid-level providers and other members of the interdisciplinary team contribute to each patient's medical record to paint a comprehensive picture of the patient's status along with any care that has been rendered. The patient's chart needs to contain enough pertinent data to enable each member of the healthcare team to render care in an integrated manner.
How to avoid referring to patients as drug seekers?
Try to avoid referring to patients as ' drug see kers,' 'rude,' 'vulgar,' 'profane,' or 'crazy' when documenting. Utilize objective phrases and direct quotes whenever possible such as ' Patient states to this writer, "You are a ___ (B-Word) and I will kill you!" '
What is medical record?
The medical record is a group of documents that should provide a comprehensive view of the patient's condition. Conversely, the medical record is not appropriate for criticizing care performed by other members of the healthcare team.
Can a nurse chart an incident report?
Never document the preparation of an incident report in the nurses notes. The incident report is an internal document meant to facilitate improvement of systems and processes within the healthcare facility. If a nurse charts a note describing that an incident report was completed, this internal form now becomes subject to discovery by external medical malpractice lawyers if legal action were to arise at a future time.
Should a nurse document a chart?
Most nurses have probably heard the old adage, " If it was not charted, it was not done !" However, some types of documentation should not be entered onto the patient's medical record for various reasons. Since the chart is a permanent record that is subject to entrance in court-ordered legal actions, nurses and other healthcare professionals must exercise extreme caution when documenting. The following is a very general list of the notations that nurses should not document in the chart.
What Is a Patient Care Report?
We often hear of care reports based on by medical teams or by medical authorities. Yet, we are not sure how this differs from the kind of report that is given to us by the same people. So this is the time to make it as clear as possible.
How to Write a Patient Care Report?
Where do you even begin when you write a patient care report? A lot of EMS or EMTs do know how to write one since they are trained to do so.
What is a patient care report?
A patient care report is a document made mostly by the EMS or EMTs. This documented report is done after getting the call. This consists of the information necessary for the assessment and evaluation of a patient’s care.
What should not be written in a patient care report?
What should be avoided in a patient care report is making up the information that is not true to the patient. This is why you have to be very careful and very meticulous when writing these kinds of reports. Every detail counts.
Who is in charge of reading the patient care report?
The person or the people who will be reading the report are mostly medical authorities. When you are going to be passing this kind of report, make sure that you have all the information correctly. One wrong information can cause a lot of issues and problems.
Popular Posts:
- 1. allergy partners oro valley patient portal login
- 2. ddoctor verma gastro patient portal
- 3. dr wilking patient portal
- 4. patient portal md synergy
- 5. patient portal south hills
- 6. dr rao patient portal
- 7. how to sign up for the sunlife patient portal
- 8. north reading medical patient portal
- 9. patient portal dr. kansikar
- 10. union hospital dover, ohio patient portal