COPD X-ray: What it looks like and diagnosis - Medical …
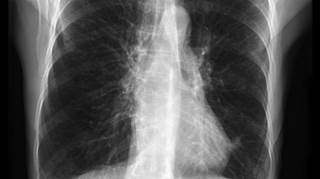
35 hours ago · COPD – bullous emphysema. Bullous emphysema manifests on a chest X-ray with areas of low density (black) with thinning of the pulmonary vessels, predominantly affecting the upper zones. The lower part of the lungs may appear denser (whiter) in normal subjects because of overlying breast tissue, but in this individual the pulmonary vessels appear normal in this area. >> Go To The Portal
How can chest X-rays help diagnose COPD?
A chest X-ray will show significant signs of COPD with the following abnormalities: Lungs become enlarged, which is termed as hyperinflation. ... Certain structural changes often occur with COPD. ... Another obvious change is the shape of the heart, which will become narrowed or appear elongated in shape due to the inflated lungs. Bullae or pockets of air begin to appear within the lungs. ...
Does COPD show up on a chest xray?
While a chest x-ray may not show COPD until it is severe, the images may show enlarged lungs, air pockets (bullae) or a flattened diaphragm. A chest x-ray may also be used to determine if another condition may be causing symptoms similar to COPD. See the Safety section for more information about x-rays. Read more
Is chest pain a sign of COPD?
This exertion can result in lower energy levels and feeling tired all the time. Chest pain and tightness are potential symptoms of COPD. Because their lungs are not functioning normally, people with COPD are more likely to experience chest infections, including the common cold, flu, and pneumonia.
What can you tell from a chest X ray?
When this happens, the healthcare provider will be able to see several things on the X-ray: 1
- A flattening of the diaphragm as the lungs press down on the muscle
- Increased chest size as measured from front to back
- An elongated and narrow heart
- Pockets of air called bullae around a half inch in size or larger

How to diagnose COPD?
To make an accurate diagnosis of COPD, a comprehensive evaluation would be performed to provide a baseline assessment of your current health, your family history, your smoking status, and any environmental or occupational toxins you may have been exposed to.
What is the purpose of chest X-rays?
If your doctor suspects you have chronic obstructive pulmonary disease (COPD), you will be likely be asked to have a chest X-ray. A chest X-ray is a simple, non-invasive imaging technique that uses electromagnetic waves to create a one-dimensional picture of your heart, lungs, and diaphragm.
What tests are used to determine how much oxygen is in the blood?
Arterial blood gasses to determine how much oxygen and CO2 is in your blood. Pulmonary function tests to measure how well your lungs inhale and exhale and how efficiently they transfer oxygen to the blood. Bronchoscopy using a flexible, lighted scope to visually examine the lung.
What are the features of a X-ray?
When this happens, the doctor will be able to see several things on the X-ray: 1 . A flattening of the diaphragm as the lungs press down on the muscle.
What is a bronchoscopy?
Bronchoscopy using a flexible, lighted scope to visually examine the lung. Pulse oximetry to measure the oxygen saturation in your blood. Six-minute walk test to assess your respiratory response to exercise.
What is the difference between a chest X-ray and a CT scan?
Where a chest X-ray will only deliver a one-dimensional image of the lungs, a CT scan will take a series of images to create a more three-dimensional representation. In doing so, the CT scan can pick up finer detail and provide doctors a more complete portrait of the person's COPD.
Is chest X-ray normal?
In early-stage disease, a chest X-ray may, in fact, appear quite normal. This doesn't mean that there is no damage; it is simply that the test has limitations as to how much it can visually tell us. It can neither describe your individual lung capacity nor the force by which you can inhale or exhale air.
What test is done to determine if you have COPD?
If your doctor suspects you may have COPD, you will likely go through a few different tests to help make a diagnosis. One of them is a chest X-ray.
Why do doctors do chest X-rays?
A chest X-ray is often done first because it is fast and accessible and provides useful information in order to make decisions quickly about your care.
What are the different types of COPD?
An easy way to think about the stages are as follows. There are also variations within the grading system: 1 Group 1 A. Mild COPD with a FEV1 of about 80 percent of normal. Few symptoms in daily life and few flare-ups. 2 Group 2 B. Moderate COPD with a FEV1 of between 50 and 80 percent of normal. 3 Group 3 C. Severe COPD with a FEV1 of between 30 and 50 percent of normal. 4 Group 4 D. Very severe COPD with a FEV1 less than Stage 3 or with the same FEV1 as Stage 3, but with low blood oxygen levels, too. Symptoms and complications of COPD significantly affect quality of life.
What is the most common COPD condition?
The most common COPD conditions are emphysema and chronic bronchitis. Emphysema is a disease that injures the small air sacs in the lungs. Chronic bronchitis is a disease that causes the airways to be constantly irritated ...
Why are bullae not seen on chest xrays?
These are typically not seen on a chest X-ray because of their small size. If a bullae or bleb ruptures, air can escape out of the lung causing it to collapse. This is known as a spontaneous pneumothorax, and it requires urgent medical treatment.
How many stages of COPD are there?
COPD is commonly separated into four stages: mild, moderate, severe and very severe. The stages are determined based on a combination of lung function and symptoms. A number grade is assigned based on your lung function, the higher the number the worse your lung function.
What is a CT scan for breathing?
A computed tomography (CT) scan of the chest is another tool that is commonly ordered in people with breathing problems. Unlike a standard X-ray, which provides a flat, one-dimensional picture, CT scans provide a series of X-ray images taken from different angles.
Why Am I Getting COPD Chest X-Rays?
If you have chronic obstructive pulmonary disease (COPD), you may wonder why your doctor occasionally asks for an X-ray of your chest.
Why do you need a high resolution CT scan for COPD?
This test can also suggest the alpha-1 antitrypsin deficiency, as condition that increases the chance to develop COPD.
What is excessive air in the lungs?
Excessive air in the lungs — abnormal collections of air in the lungs medically known as focal bullae.
How to take a front view of an X-ray?
During the front view, remember to stand against the plate, hold your arms up (or to the side), roll your shoulder forward and take deep breaths when you are asked to — this way the image will be clearer.
Does COPD show changes?
However, as the disease progresses, it may show changes associated with COPD. These include:
What grade should a chest X-ray be for COPD?
The BTS/NICE COPD guideline recommends a chest X-ray at initial COPD evaluation; this is a grade D recommendation based on expert opinion. We have investigated which pathologies other than COPD are detected by chest X-ray and how they alter management. Dundee smokers aged 40 or over and receiving bronchodilators are assessed for COPD by their practice nurse and offered a chest X-ray if there is no record of a chest X-ray within the previous three years. We retrospectively analysed the chest X-ray reports and case records of these patients. The chest X-ray report was structured with 7 specific questions, most importantly "Are there any features of other disease likely to be causing dyspnoea?" and "Are there any features to suggest lung cancer?" Management of patients with chest X-ray findings suggesting other disease causing dyspnoea or lung cancer was assessed by questionnaire and case record study. Five hundred forty-six consecutive chest X-ray reports were analysed. Fourteen percent of all chest X-rays detected potentially treatable dyspnoea causing disease; where management following receipt of X-ray reports was audited, 84% were thought to help. Eleven lung cancers were detected, 3 had stage 1 disease. Considerable benign and malignant pathology is detected by chest X-ray performed at initial COPD assessment. Clinical management is changed in the majority with a potentially treatable abnormality. This evidence suggests that the NICE guideline to perform chest X-ray at initial COPD evaluation should be elevated from a grade D to grade C recommendation.
Is a chest X-ray grade D?
The BTS/NICE COPD guideline recommends a chest X-ray at initial COPD evaluation; this is a grade D recommendation based on expert opinion. We have investigated which pathologies other than COPD are detected by chest X-ray and how they alter management. Dundee smokers aged 40 or over and receiving br …
What is COPD spirometry?
While spirometry is a very useful diagnostic tool for screening large groups of smokers , it cannot readily differentiate the etiologies of COPD and thus has limited utility in characterizing subjects for clinical and investigational purposes. There has been a longstanding interest in thoracic imaging and its role in the in-vivo characterization of smoking related lung disease. Research in this area has spanned readily available modalities such as chest x-ray and computed tomography to more advanced imaging techniques such as optical coherence tomography and magnetic resonance imaging. While chest x-ray is almost universally available, it lacks sensitivity in detecting both airway disease and mild emphysema, and is not generally amenable to objective analysis. Computed tomography has become the standard modality used for objective visualization of disease. It can provide useful measures of emphysema, airway disease, and more recently pulmonary vascular disease for clinical correlation. It does, however, face limitations in standardization across brands and generations of scanners, and the ionizing radiation associated with image acquisition is of concern to both patient and health care provider. Newer techniques such as OCT and MRI offer exciting in-vivo insight into lung structure and function that was previously available only in necropsy specimens and physiology labs. Given the more limited availability of these techniques, they are at present viewed as adjuncts to CT imaging.
How to detect emphysema on CT?
These can be preliminarily divided into two categories, visual detection schemes and more objective techniques based upon lung density. Typically, subjective approaches to analysis such as visual interpretation involve either a global or regional assessment of the lung using an ordinal scoring system (i.e. 0–4) to reflect disease severity. Using visual interpretation schemes, multiple investigators have demonstrated a correlation to histopathology (9–12), lung function (13, 14), and even response to therapeutic intervention.(3) Limitations to these approaches are, however, their susceptibility to intra and inter-observer variability (15), sensitivity to the viewing conditions such as window width and level (16, 17), and potential insensitivity for the detection of disease progression in longitudinal studies. Paradoxically, a potential strength to such analysis is that same ability of the user to be either consciously or unconsciously influenced by their visual perception of disease. Depending on the experience of the user, subtle patterns of disease may be observed that are not readily amenable to objective quantification.
What is the site of expiratory airflow obstruction in smokers?
The site of expiratory airflow obstruction in smokers is believed to be the peripheral small airways.(31) While the size of these airways precludes their direct assessment on clinical CT scans, recent investigation has demonstrated that the morphology of the central cartilaginous airways reflect the distal remodeling process. In 2000, Nakano and colleagues demonstrated that in smokers, subjects with the greatest degree of mural thickening and lumenal occlusion of the apical segment of the right upper lobe tended to have the lowest FEV1expressed as a percent of predicted (32) and a greater burden of distal small airway disease on histopathologic examination.(33) Further, the combination of CT measures of emphysema and densitometric measures of emphysema provided additive information when predicting lung function. Interestingly, there was no relationship between absolute airway wall thickness and lung function which alludes to the overall variability native airway morphology in this group. To address this issue investigators employed a measure called the Wall Area Percent (WA%) which is calculated as 100 times the airway wall area divided by the total bronchial cross sectional area.(32) This has become the standard CT based measure of airway disease in smokers.
What are the limitations of CT scans?
Such systematic issues can bias data so that subjects at a given center may appear to have more or less emphysema for a given degree of tobacco smoke exposure or expiratory airflow obstruction. A second well documented limitation of quantitative CT scan analysis is the resolution imposed by clinical imaging protocols. Standard theory in image analysis states that structures smaller than 2 pixel widths in size cannot be resolved with accuracy. (53) Since the wall thicknesses of the 4thand 5thgeneration airways tend to fall in this range, consideration must be given to the accuracy of such measures prior to clinical application despite their providing a more robust biologic signal.
What is bronchiectasis on a CT scan?
Bronchiectasis is characterized radiographically as the abnormal dilation of the airway lumen with concomitant wall thickening.( 39, 40) Its prevalence in the general population of smokers with COPD is unknown. In one of the largest reported CT based studies of smokers to date, Patel and colleagues found that approximately 2.5% of subjects had moderate to severe disease.(41) In contrast, Parr and colleagues found that almost 95% of their study cohort of subjects with AATD exhibited some bronchiectatic changes in their airways.(42) There are 2 notable differences to these studies. The first is that the prevalence estimate published by Parr and colleagues included subjects with even mild, regionally limited disease while those estimates reported by Patel and colleagues were based on severe disease that precluded quantitative airway analysis. The second is related to the unique pulmonary manifestations of smoking related lung disease in smokers with or without AATD. Further investigation is needed to determine the prevalence and clinical associations of bronchiectatic airway disease detected on CT scan in smokers.
What are contrast agents used for MRI?
Some of the newest and most exciting agents under investigation are the hyperpolarized noble gases such as helium (3He) and xenon (129Xe). While both gases provide detailed images of the tracheobronchial tree and allow global and regional measurement of surface to volume ratio(65, 66), 129Xe has the added property of being diffusible across the alveolar capillary membrane and can therefore be used to examine the septal thickness and diffusion capacity.(66–68) Further work is needed using these and other contrast agents however such techniques may truly allow in-vivo assessment of lung function in both health and disease.
What is CT measure of airway disease?
To this point, CT measures of airway disease have been defined as mural thickening with encroachment on the lumen. While useful for functional correlation, their relationship to another clinically significant occurrence, acute exacerbations of COPD, is currently undefined. In contrast, another radiographic form of airway disease, bronchiectasis, is increasingly being recognized for its association with elevated biomarkers of inflammation and the severity of respiratory events.(38)
When was the retrospective analysis of COPD chest X-rays done?
A retrospective analysis of all COPD screening chest X-ray reports for a two-year period from June 2003 until May 2005 was performed by one observer. Following this, case notes were reviewed of all patients found to have screening chest X-rays suggestive of lung cancer. Questionnaires were sent to the appropriate COPD practice nurse regarding ...
How many patients with COPD have lung cancer?
Lung cancer was confirmed in 9 of 14 patients with COPD and radiological features suggesting this diagnosis on their X-ray. In addition the diagnosis of lung cancer followed a repeat film in 2 of 27 patients in whom a repeat chest X-ray was recommended because of consolidation on the screening chest X-ray. Thus 49.6 chest X-rays were performed to detect 1 lung cancer. The stage and pathology of the carcinomas and treatment given are shown ( Table 4 ). Five patients had potentially curative treatment with 4 of them having surgery. This compares favourably with the local surgical resection rate of 8%.
What are the abnormalities other than lung cancer?
Abnormalities other than lung cancer believed to be causing dyspnoea are shown in Table 2 and those unlikely to be causing dyspnoea are shown in Table 3. Of the 106 patients, 76 had potentially treatable disease, namely 51 with lower respiratory tract infection, 8 with bronchiectasis, 6 with pulmonary fibrosis, 4 with pleural effusion, 4 with left ventricular failure, and 3 with possible active TB. Thus 14% of all chest X-rays requested at COPD evaluation detected potentially treatable causes of dyspnoea other than lung cancer and COPD.
What grade should a chest X-ray be?
The BTS/NICE COPD guideline recommends a chest X-ray at initial COPD evaluation; this is a grade D recommendation based on expert opinion. We have investigated which pathologies other than COPD are detected by chest X-ray and how they alter management. Dundee smokers aged 40 or over and receiving bronchodilators are assessed for COPD by their practice nurse and offered a chest X-ray if there is no record of a chest X-ray within the previous three years. We retrospectively analysed the chest X-ray reports and case records of these patients. The chest X-ray report was structured with 7 specific questions, most importantly “Are there any features of other disease likely to be causing dyspnoea?” and “Are there any features to suggest lung cancer?” Management of patients with chest X-ray findings suggesting other disease causing dyspnoea or lung cancer was assessed by questionnaire and case record study.
How many people in the UK have COPD?
The burden of disease from chronic obstructive pulmonary disease (COPD) is large. It is estimated that up to 1.5 million of the UK population have COPD but the exact prevalence is unknown.1 The extent of coexisting respiratory disease other than COPD is also unknown. The National Institute for Health and Clinical Excellence (NICE) ...
How many patients were given antibiotics after a chest xray?
Lower respiratory tract infection was not suspected in 28 patients prior to their X-ray. Twenty-seven of these were given antibiotics after the X-ray and 24 of the 27 in whom a follow-up chest X-ray was recommended underwent one.
How many questions are asked on a structured chest X-ray report?
Table 1. The 7 questions on the structured chest X-ray report.
What is an exacerbation of COPD?
The Global Initiative for Chronic Obstructive Lung Disease (GOLD) guideline defines a COPD exacerbation as “an acute worsening of respiratory symptoms that result in additional therapy” [1]. This definition contains two components: the need for a change in symptoms, and for that change in symptoms to result in additional therapy. A major criticism of the GOLD definition is that it does not reflect clinical practice: there are many causes of symptom changes in a patient with COPD that need additional therapy that are not considered COPD exacerbations—heart failure, pneumothorax and pulmonary embolus to name three. In the absence of a biomarker that can reliably differentiate exacerbation of COPD from baseline COPD [2], or exacerbation of COPD from other causes of symptom deterioration, in clinical practice an exacerbation is therefore considered a clinical diagnosis of exclusion—made when other causes of symptoms changes have been considered and where appropriate excluded through investigation [3].
What is the best treatment for COPD exacerbation?
Standard therapy for a COPD exacerbation includes an increase in dose and/or frequency of short-acting bronchodilators, short-course oral corticosteroids and antibiotics when there has been a change in sputum [1]. It is important to provide appropriate support for ventilatory failure, and to attend to co-morbidities. Standard therapy for community-acquired pneumonia, outside the context of COPD, would usually comprise antibiotics to cover typical and atypical pathogens (for example a beta-lactam and macrolide combination). Whilst viruses are a common cause of COPD exacerbations, as described above, Huerta [14] did not isolate respiratory viruses in their sample of 55 exacerbations with consolidation, in which the commonest pathogen isolated was Streptococcus pneumoniae(in 43% of cases). The most common bacterial pathogen in the patients without consolidation was Haemophilus influenzae.
What causes COPD exacerbation?
Our current understanding of a COPD exacerbation is that the airway inflammation that characterises COPD is further increased by stimuli such as respiratory viruses and alterations in the airway bacterial flora, resulting in bronchoconstriction, mucus plugging and ventilation-perfusion mismatch that cause the characteristic symptoms of additional breathlessness, sputum and wheeze [4]. A COPD exacerbation is therefore predominantly driven by airway, rather than alveolar infection. We know that viruses are important causes of COPD exacerbations from epidemiological studies [5], and experimental studies using human rhinovirus [6]. Understanding how alterations in bacterial flora associate with exacerbation is more complex in the era of the microbiome, but likely includes a reduction in community diversity. It is also likely that airway bacteria and viruses interact [7]. Lastly, there are epidemiological data supporting the concept that COPD exacerbations may be caused by pollutants [8].
What percentage of COPD patients have a consolidation?
Twenty percent of chronic obstructive pulmonary disease (COPD) patients admitted to hospital because of an ‘exacerbation’ will have consolidation visible on a chest X-ray. The presence of consolidation is associated with higher mortality. Imperfect definitions of COPD exacerbation and pneumonia, and incomplete and imperfect diagnostic tests, have resulted in a debate about whether these episodes are best thought of as ‘exacerbation with consolidation’ or ‘pneumonia in a person with COPD’. With the current views that exacerbations are not all identical, and that they can be ‘phenotyped’ to identify episodes with different prognosis and treatment response, perhaps these episodes are best-considered a phenotype of exacerbation. Whatever the terminology, the important clinical message is to recognise that those with consolidation have higher mortality, and likely different responses to treatment.
Does CT scan show COPD?
Increasingly, patients admitted to hospital with COPD undergo computed tomography (CT) scanning. It is not clear, at present, whether the presence of consolidation on CT has the same prognostic significance as consolidation on chest X-ray (CXR), but a recent study has reported that a serum CRP cutoff of 11.5 mg had a sensitivity of 91% and a specificity of 53% for CT consolidation [17].
Is chest X-ray a part of routine care?
Because a chest X-ray is not part of routine care for most community-treated COPD exacerbations, the prevalence of consolidation at the time of a COPD exacerbation is unknown. There are data looking at the presence of consolidation in hospitalised exacerbations, but it is important to note that an exacerbation presenting to hospital, a ‘severe exacerbation’, is characterised by a more severe presentation which can arise from severe underlying COPD and/or a severe additional insult, or the presence of co-morbidities and/or a lack of social support.
Does COPD have consolidation?
A number of studies have examined differences between patients presenting with COPD deteriorations with and without consolidation. Huerta and colleagues [14] recruited 249 consecutive admissions to hospital with COPD, 116 of whom had consolidation. Chills, pleuritic chest pain and sputum purulence were the symptoms that best predicted consolidation, and those with consolidation also had elevated systemic inflammation as assessed by C-reactive protein (CRP, 17 vs. 7 mg/L), but milder underlying disease (higher forced expiraroty volume (FEV1)). Markers of systemic inflammation remained higher in those with consolidation.